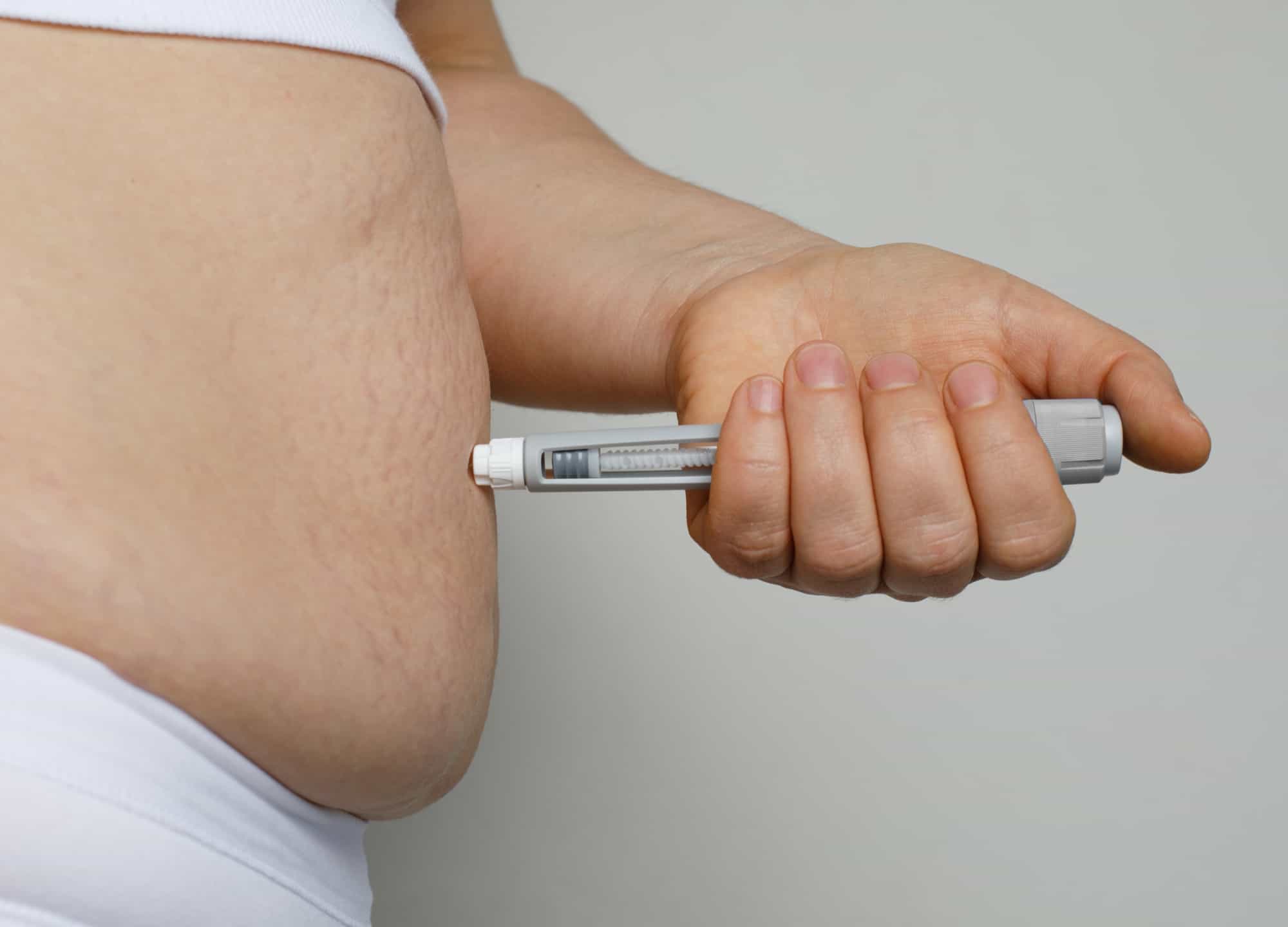
Semaglutide Weight Loss Program in Southlake, TX
Semaglutide isn't a shortcut — it's a clinically validated GLP-1 agonist that fundamentally changes how your brain processes hunger. Dr. Farhan Abdullah manages your semaglutide program in Southlake with real lab monitoring, dose titration, and the kind of physician oversight that a weight loss spa simply can't provide.
Learn More About
Semaglutide
What is
Semaglutide
Semaglutide is a GLP-1 (glucagon-like peptide-1) receptor agonist — a synthetic analog of the naturally occurring incretin hormone GLP-1, engineered with a fatty acid side chain that extends its half-life to approximately one week, enabling once-weekly subcutaneous injection. It's FDA-approved under the brand name Ozempic for type 2 diabetes management and Wegovy for chronic weight management in adults with obesity (BMI ≥30) or overweight (BMI ≥27) with at least one weight-related comorbidity.
GLP-1 is an incretin hormone secreted by L-cells in the small intestine in response to nutrient intake. Its natural physiologic actions include stimulating glucose-dependent insulin secretion, suppressing glucagon release, slowing gastric emptying, and signaling satiety to the hypothalamus. Semaglutide activates GLP-1 receptors throughout the body — in the pancreas, gut, and critically in the brain, particularly in the hypothalamic arcuate nucleus and reward-processing regions of the mesolimbic system. This central nervous system activity is what produces the reduction in appetite, food cravings, and the subjective preoccupation with food that many patients describe as "food noise" — the background mental chatter about eating that semaglutide substantially quiets.
The STEP 1 trial (Wilding et al., NEJM 2021) demonstrated an average 14.9% body weight reduction with semaglutide 2.4mg weekly over 68 weeks, compared to 2.4% with placebo — a magnitude of effect that no prior anti-obesity medication had achieved. The SELECT cardiovascular outcomes trial published in 2023 added a cardiovascular benefit signal: semaglutide reduced major adverse cardiovascular events by 20% in overweight and obese patients with established cardiovascular disease, independent of diabetes status. These aren't marketing claims — they're peer-reviewed outcomes data from large randomized trials.
Why do We Use
Semaglutide
Obesity is a chronic disease with a neurobiological basis — the hypothalamic and reward system dysregulation that drives excess caloric intake and fat accumulation isn't a character defect, and it doesn't respond reliably to willpower-based interventions alone. Semaglutide addresses the neurobiology directly: GLP-1 receptor agonism in the arcuate nucleus suppresses appetite signaling, and mesolimbic GLP-1 receptor activity reduces the reward salience of food that drives compulsive and excess eating.
The clinical evidence behind semaglutide is exceptional by any standard in medicine. The STEP trials represent some of the largest and most rigorous weight loss intervention trials ever conducted, with outcomes that exceed what bariatric surgery achieved in trials a decade ago. SELECT's cardiovascular endpoint data elevated semaglutide from a weight management medication to a cardiovascular risk reduction tool. This is a pharmacologically and clinically serious medication — which is why physician supervision matters.
Unsupervised telehealth prescribing of semaglutide without metabolic evaluation, without addressing the hormonal contributors to weight gain, and without structured dose titration produces variable results and misses the clinical opportunity. Dr. Abdullah evaluates thyroid function, testosterone (in men), insulin resistance markers, and the full metabolic picture before starting semaglutide — because a man with testosterone of 200 ng/dL and obesity needs TRT alongside GLP-1 therapy for optimal results, not one treatment administered in isolation from the other.
Key Benefits of
Semaglutide
Clinically Validated 15% Average Weight Reduction: The STEP trial program produced average weight loss of approximately 15% of body weight — a magnitude that meaningfully reduces cardiovascular risk, improves glycemic control, reduces joint loading, and produces the metabolic downstream effects that lower-efficacy interventions don't generate. For context, a 15% reduction from 220 lbs is 33 lbs. That's the scale of change that moves metabolic markers, not just the number on the scale.
Reduction in Cardiovascular Risk: The SELECT trial demonstrated a 20% reduction in major adverse cardiovascular events with semaglutide in overweight and obese patients with established CVD — independent of diabetes status or the degree of weight loss achieved. The cardiovascular benefit appears to be partially independent of the weight loss itself, suggesting direct vascular and anti-inflammatory mechanisms beyond caloric reduction. For patients with cardiovascular risk factors, this is not a cosmetic medication.
Central Reduction of Food Noise and Cravings: The hypothalamic and mesolimbic GLP-1 receptor activity that semaglutide produces reduces the subjective preoccupation with food, cravings, and reward-driven eating that behavioral approaches alone struggle to override. Patients frequently describe semaglutide as the first intervention that made behavioral change feel possible — because the pharmacologic action removes the constant cognitive pull toward food that makes sustained caloric restriction so difficult without medication.
Glycemic Improvement and Diabetes Prevention: Semaglutide's glucose-dependent insulin secretion stimulation and glucagon suppression improve postprandial glycemic control regardless of diabetes status. For patients with prediabetes or insulin resistance driving weight gain and metabolic dysfunction, semaglutide addresses the glycemic component while producing weight loss that further improves insulin sensitivity — a compounding metabolic benefit.
Once-Weekly Dosing — Practical Adherence: The one-week half-life of semaglutide enables once-weekly subcutaneous injection rather than daily administration, which significantly improves adherence compared to daily injection protocols. For most patients, the injection becomes a brief weekly routine rather than a daily obligation.
Who Benefits Most From
Semaglutide
Patients with BMI 27–35 and Weight-Related Comorbidities: Semaglutide's FDA approval for chronic weight management at BMI ≥27 with a comorbidity covers a substantial proportion of overweight adults who've been told they don't qualify for obesity treatment. Hypertension, dyslipidemia, prediabetes, obstructive sleep apnea, and osteoarthritis are all qualifying comorbidities — and all of them improve meaningfully with 10–15% weight reduction. This is the core population where semaglutide's risk-benefit profile is well-characterized and the clinical rationale is straightforward.
Patients Who've Failed Lifestyle Intervention: Sustained caloric restriction fails the majority of people who attempt it long-term — not because of inadequate motivation, but because the hypothalamic weight-defense mechanisms that evolved to protect against starvation actively counteract weight loss, increasing appetite and reducing metabolic rate in response to caloric deficit. Semaglutide suppresses these homeostatic defense mechanisms at the receptor level, making sustained caloric deficit pharmacologically achievable for patients who've demonstrated through repeated attempts that behavioral approaches alone aren't sufficient.
Men with Obesity and Low Testosterone: Visceral adiposity drives aromatase activity that converts testosterone to estrogen, suppressing pituitary LH secretion and producing secondary hypogonadism. Men with significant abdominal obesity and low testosterone are caught in a cycle where low testosterone promotes fat accumulation and fat accumulation further suppresses testosterone. Semaglutide breaks the cycle on the weight side; TRT addresses the hormonal side. The combination produces results that neither intervention achieves independently — a clinical synergy Dr. Abdullah manages specifically for this population.
Patients with Prediabetes or Early Insulin Resistance: The window between insulin resistance and frank type 2 diabetes is the highest-leverage intervention point in metabolic medicine — changes made here prevent a chronic disease rather than managing one that's already established. Semaglutide's glucose-dependent insulin secretion support and weight-loss-driven insulin sensitivity improvement address prediabetes from two angles simultaneously, with a meaningful probability of preventing progression to diabetes altogether.
Patients Seeking Sustained Weight Loss Before Transitioning Off Medication: A common patient concern is medication dependency — needing to stay on semaglutide indefinitely to maintain results. This is a legitimate clinical consideration. Patients who use semaglutide as a pharmacologic bridge to establish new behavioral patterns, improve metabolic health, and reduce fat mass can sometimes transition to lower doses or off medication with sustained results, particularly when the foundational hormonal and metabolic picture has been optimized. Dr. Abdullah discusses transition planning as part of the initial program design.
What To Expect From
Semaglutide
Step 1 — Comprehensive Metabolic Evaluation: Labs including thyroid panel, testosterone (men), fasting insulin, HbA1c, lipids, CBC, and metabolic panel establish the metabolic picture driving your weight before any medication is prescribed. This isn't an intake form — it's a clinical evaluation that determines whether semaglutide is the right primary intervention and what needs to be addressed alongside it.
Step 2 — Starting Dose and Titration Schedule: Semaglutide starts at 0.25mg weekly for the first 4 weeks — a ramp-up dose designed to establish GI tolerance rather than produce weight loss. The dose increases every 4 weeks through 0.5mg, 1mg, and 1.7mg to the full maintenance dose of 2.4mg (Wegovy) or as clinically indicated based on your response and tolerability. The titration schedule exists to manage nausea and GI side effects — rushing it produces unnecessary discomfort without clinical benefit.
Step 3 — Injection Training: Semaglutide is a once-weekly subcutaneous injection into the abdomen, thigh, or upper arm. Our clinical team walks through injection technique at your first visit. The pen devices are straightforward; most patients are comfortable after a single demonstration.
Step 4 — Ongoing Monitoring: Follow-up visits at 4–8 week intervals to assess weight loss rate, side effect profile, and metabolic marker response. Labs are repeated at intervals appropriate to your clinical picture. Dose adjustments are made based on objective response — not a rigid predetermined schedule.
Step 5 — Nutritional and Behavioral Integration: Semaglutide reduces appetite and food noise — it doesn't replace nutrition. Our team provides guidance on protein intake optimization (critical for maintaining lean mass during GLP-1-driven weight loss), hydration, and the behavioral patterns that compound the pharmacologic effect. Patients who maintain adequate protein intake preserve lean mass significantly better than those who don't.
Is
Semaglutide
right for me?
Semaglutide is appropriate for adults with BMI ≥30, or BMI ≥27 with a weight-related comorbidity, who haven't achieved adequate results with lifestyle intervention alone and don't have contraindications. The primary contraindications are a personal or family history of medullary thyroid carcinoma or multiple endocrine neoplasia syndrome type 2 (MEN2) — based on thyroid C-cell tumor findings in rodent studies at suprapharmacologic doses, with no established causation in humans at clinical doses but a sufficient concern for the contraindication to stand. Active pancreatitis is also a contraindication.
GI side effects — nausea, vomiting, constipation, diarrhea — are the primary tolerability concerns and are managed through careful dose titration. Most patients experience significant GI symptoms during the first 4–8 weeks that diminish substantially as tolerance develops. Patients who rush the titration or skip meals while on semaglutide tend to have worse GI tolerability.

🏆 Voted "Best in Tarrant County" by Society Life Magazine (2023-2025)
Semaglutide Weight Loss Program — Southlake, TX
The STEP trial results were the kind of data that don't come along often in medicine: 14.9% average body weight reduction over 68 weeks in a large randomized controlled trial. Then the SELECT cardiovascular outcomes trial added a 20% reduction in major adverse cardiovascular events in overweight and obese patients with established heart disease — independent of diabetes status, and partially independent of the weight loss itself. That's not a weight loss supplement. That's a cardiometabolic medication with Level 1 evidence.
At Magnolia Functional Wellness, Dr. Farhan Abdullah manages semaglutide as exactly that — a serious pharmacologic tool within a clinically structured program, not a prescription dispatched from a telehealth queue.
The Program: Structure, Titration, and Follow-Up
Semaglutide at Magnolia starts at 0.25mg weekly and increases every 4 weeks through the 2.4mg maintenance dose — a 16–20 week titration designed to give your GI system time to adapt and minimize the nausea, vomiting, and constipation that rushing produces. Follow-up visits at 4–8 week intervals track weight loss rate, metabolic marker response, and lean mass preservation. Protein guidance is provided at initiation because GLP-1-driven appetite suppression reduces caloric intake broadly — without adequate protein (typically 1.2–1.6g per kg body weight), you lose muscle alongside fat, and that's both metabolically and aesthetically wrong.
Transition planning is part of the program from day one. Weight regain after stopping is real, documented in the STEP 4 trial, and expected when the biology of obesity isn't also addressed. Dr. Abdullah builds hormonal and metabolic optimization into the program so that when the time comes to consider stepping down, the foundation under the weight loss is actually stable.
Premium Care, Honest Pricing
We are proud to offer the lowest price for medically supervised GLP-1 therapy in Southlake.
How? Unlike corporate medspas with high overhead and franchise fees, Magnolia Functional Wellness is an independent medical practice. We believe life-changing weight loss should be accessible. You get the highest standard of Internal Medicine care—without the "luxury markup."
Serving Southlake and the Greater DFW Area
We serve patients from Southlake, Westlake, Grapevine, Keller, Colleyville, Flower Mound, Trophy Club, and across the Dallas-Fort Worth Metroplex. Telehealth follow-up is available for established patients. Both branded Wegovy/Ozempic and compounded semaglutide options are discussed at consultation based on current access and your clinical situation.
How Process Works at
Magnolia Functional Wellness
Assess
We begin with a comprehensive evaluation of your health, goals, and medical background to understand the root causes, not just the symptoms.
Personalize
Based on your results, we create a tailored functional wellness plan using evidence-based therapies designed specifically for your body and needs.
Optimize
Through ongoing care, monitoring, and adjustments, we help you achieve sustainable improvements in performance, vitality, and long-term health.
STEP Trial Evidence — 15% Average Weight Reduction
The semaglutide STEP trial program produced some of the most impressive weight loss outcomes ever documented in a pharmaceutical trial — average 14.9% body weight reduction at 68 weeks. This isn't a supplement with equivocal evidence; it's a medication with Level 1 randomized controlled trial data across tens of thousands of patients.
SELECT Cardiovascular Outcomes Data — Not Just a Weight Loss Drug
The SELECT trial demonstrated a 20% reduction in major adverse cardiovascular events with semaglutide in overweight and obese patients with established CVD. The cardiovascular benefit appears partially independent of weight loss magnitude. For patients with cardiovascular risk factors, semaglutide is a risk reduction medication, not just a weight management tool.
Structured Titration That Manages Side Effects Properly
The GI side effects of semaglutide are largely titration-rate dependent. Dr. Abdullah follows a structured dose escalation protocol — starting at 0.25mg and increasing every 4 weeks — that gives your GI system time to adapt. Patients who rush titration outside of physician supervision tend to have worse tolerability and higher discontinuation rates.
Integration with TRT, GLP-1 Alternatives, and Longevity Protocols
Men with obesity and low testosterone need both conditions addressed simultaneously for optimal results. Patients who plateau on semaglutide have a clear path to tirzepatide or retatrutide. Patients on longevity protocols benefit from the visceral fat reduction and metabolic improvement that semaglutide produces alongside their other interventions. Everything is managed within the same clinical relationship at Magnolia.
Transition Planning from the Beginning
Weight regain after stopping GLP-1 medications is real. Dr. Abdullah builds transition planning into the program from the start — using the medication course to optimize the hormonal and metabolic foundation, establish behavioral patterns, and evaluate candidacy for maintenance or step-down protocols. The goal is sustainable metabolic health, not indefinite medication dependency.
Your Questions Answered
Led by trained medical professionals delivering safe, effective, and scientifically backed aesthetic and wellness treatments.
Will I regain the weight when I stop semaglutide?
Weight regain after discontinuing GLP-1 medications is real and documented — the STEP 4 trial showed meaningful regain after stopping semaglutide. This reflects the chronic disease biology of obesity: the pharmacologic suppression of weight-defense mechanisms is removed when the medication stops. Dr. Abdullah discusses this honestly and structures programs around transition planning — optimizing hormonal and metabolic health during the medication course, establishing behavioral patterns, and evaluating candidacy for maintenance dosing or transition to a lower-efficacy alternative.
Is semaglutide the same as Ozempic or Wegovy?
Yes — Ozempic and Wegovy are brand names for semaglutide at different doses. Ozempic (0.5–2mg weekly) is FDA-approved for type 2 diabetes. Wegovy (2.4mg weekly) is FDA-approved for chronic weight management. The active ingredient is identical; the approved indication and maximum dose differ. Compounded semaglutide — produced by 503B compounding pharmacies — is also available at comparable doses when branded supply is limited.
What should I expect during Semaglutide treatment?
During your semaglutide consultation and treatment at Magnolia Functional Wellness, you can expect a thorough assessment, personalized treatment plan, and physician-supervised care in a calm, clinical environment. Our team will guide you through each step and ensure you're comfortable throughout the process. Treatment duration and frequency will be discussed during your initial consultation based on your specific needs and goals.
How long does it take to see results from Semaglutide?
Results from Semaglutide at Magnolia Functional Wellness vary based on individual factors, treatment protocol, and your specific goals. Some patients notice improvements [timeframe], while others may see optimal results over [extended timeframe]. Our physician-supervised approach ensures we monitor your progress and adjust treatment as needed to achieve the best possible outcomes. During your consultation, we'll provide a realistic timeline based on your unique situation.
How is retatrutide different from semaglutide and tirzepatide?
Semaglutide (Ozempic, Wegovy) activates one receptor — GLP-1. Tirzepatide (Mounjaro, Zepbound) activates two — GLP-1 and GIP. Retatrutide activates all three: GLP-1, GIP, and glucagon. The glucagon receptor component is what distinguishes retatrutide — it drives energy expenditure at rest, promotes fat oxidation over muscle catabolism, produces dramatic liver fat reduction, and contributes to the osteoarthritis pain relief seen in clinical trials. Phase 3 data shows 28.7% average weight loss compared to approximately 15% for semaglutide and 20-21% for tirzepatide. These are not incremental differences — they represent a meaningful step change in efficacy.
Why are your GLP-1 prices lower than other Southlake clinics?
We are a physician-owned medical clinic, not a corporate medspa franchise. We don't have "middlemen" or franchise fees to pay, so we don't pass those costs on to you. You are paying for the medication and Dr. Abdullah's medical expertise—nothing else.
Need More Information?
Our team is ready to answer your specific questions and concerns.





Redefine Your Glow. Reimagine Your Life.
Led by trained medical professionals delivering safe, effective, and scientifically backed aesthetic and wellness treatments.
Not what you were looking
for? Explore More.
At Magnolia Functional Wellness, every treatment is guided by medical science, regenerative principles, and individualized care. We focus on restoring physiology at its source, enhancing vitality, and supporting long term health with evidence based interventions that go beyond traditional aesthetics.



.svg)