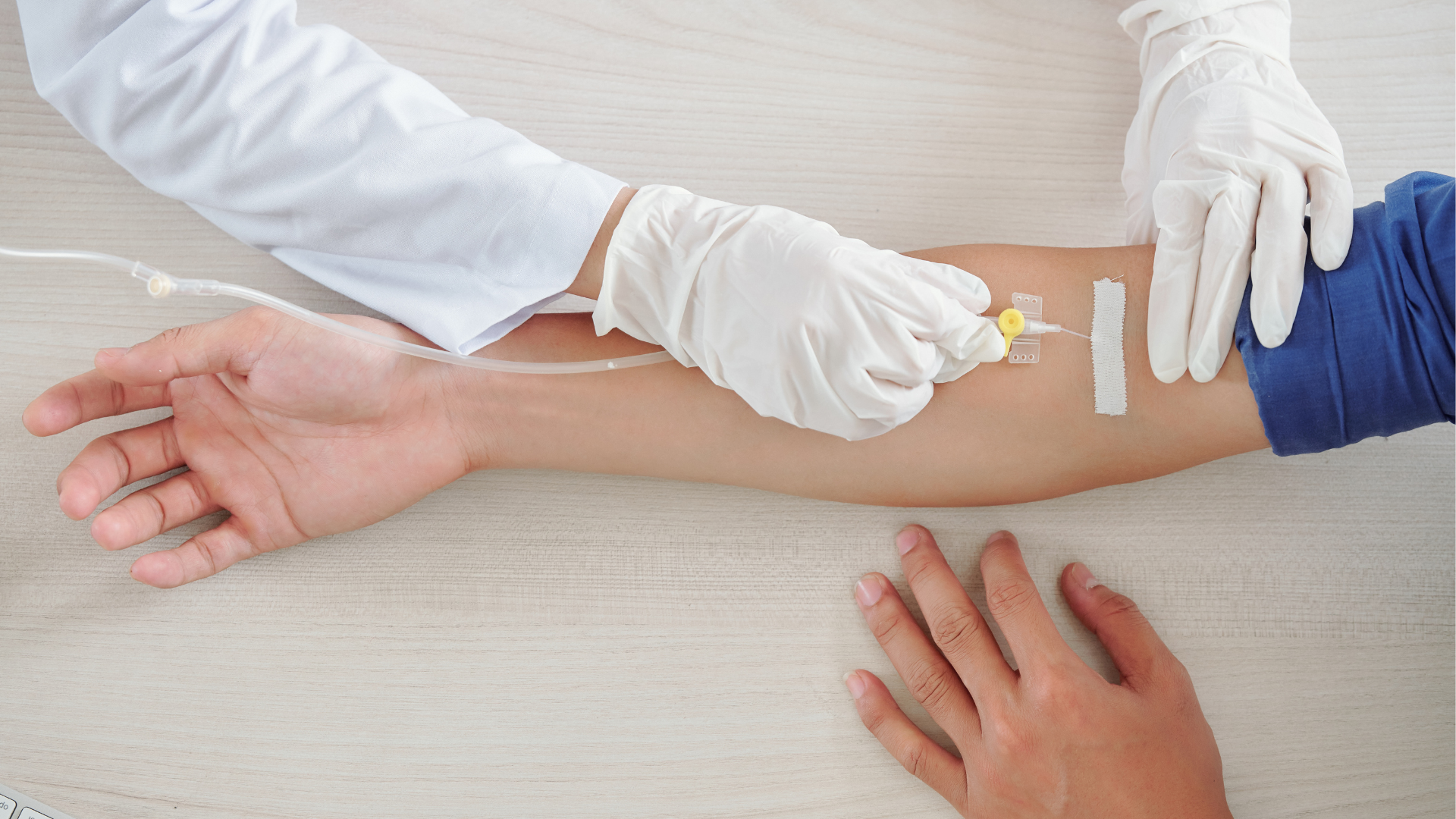
IV Iron Infusions in Southlake, TX
Iron deficiency is the most common nutritional deficiency in the world — and one of the most consequentially undertreated. For women dealing with heavy menstrual bleeding, patients who can't tolerate or absorb oral iron, or those who need IV delivery to replete stores that oral supplementation simply can't keep up with, intravenous iron is often the right answer. At Magnolia Functional Wellness, Dr. Farhan Abdullah offers physician-supervised IV iron infusions using Venofer (iron sucrose) — a well-established, non-dextran formulation with a strong safety record and decades of clinical use.
Learn More About
IV Iron Infusions
What is
IV Iron Infusions
IV iron infusion delivers elemental iron directly into your bloodstream through an intravenous catheter, bypassing the gastrointestinal system entirely. Magnolia Functional Wellness uses Venofer — the brand name for iron sucrose injection — an FDA-approved, non-dextran IV iron formulation with decades of clinical use and a well-established safety profile.
Venofer consists of an iron core surrounded by a sucrose carbohydrate shell that holds the iron in a stable, non-ionic complex until it's processed by the body's reticuloendothelial system. Once infused, the iron complex is taken up by macrophages, the sucrose shell is metabolized, and the elemental iron is stored as ferritin or bound to transferrin for delivery to the bone marrow and other tissues where it's needed.
Iron is essential for hemoglobin production, myoglobin function, energy metabolism, immune function, and neurotransmitter synthesis. When iron stores are depleted, the downstream effects are far-reaching and frequently dismissed: profound fatigue, exercise intolerance, cognitive fog, headaches, hair loss, pica (cravings for ice, dirt, or starch), restless legs syndrome, cold intolerance, and eventually frank anemia with shortness of breath. Many women live with these symptoms for months or years — attributing them to stress, sleep deprivation, or simply the demands of life — before proper lab evaluation reveals iron deficiency as the underlying cause.
Venofer is administered as a series of infusion sessions. Each session delivers 200mg of elemental iron over approximately 30 minutes. Most patients requiring full iron store repletion receive a total course of around 1,000mg — typically five sessions — scheduled at intervals Dr. Abdullah determines based on your clinical picture and response.
Why do We Use
IV Iron Infusions
The case for IV iron over oral supplementation in the right patient comes down to three things: absorption, tolerability, and pace.
Absorption: Oral iron relies on functional intestinal absorption — a process limited by saturation of intestinal transporters, gut inflammation, and hepcidin regulation. Hepcidin is a liver-produced hormone that suppresses intestinal iron uptake and is elevated by inflammation, infection, and chronic disease — precisely the conditions that often accompany iron deficiency in the patients who need repletion most. At best, 10–20% of an oral iron dose is absorbed. In patients with gut inflammation, IBD, or altered post-surgical anatomy, absorption may be considerably less. IV iron bypasses this entirely — 100% of the administered dose enters the circulation.
Tolerability: Oral iron is notoriously difficult to take at doses sufficient for meaningful repletion. Nausea, constipation, dark stools, GI cramping, and heartburn cause many patients to reduce their dose, take it inconsistently, or stop altogether — defeating the purpose and leaving the deficiency untreated. IV iron produces no GI side effects at all. For patients who have genuinely tried oral iron and found it intolerable, IV isn't a fallback — it's the appropriate solution.
Pace: A patient who has lost significant iron through heavy menstrual bleeding, chronic gut inflammation, or inadequate absorption doesn't just need iron replaced — she needs it replaced before the next cycle of loss begins. Oral supplementation at standard doses can take months to meaningfully restore ferritin levels. IV delivery, spread across a series of sessions, achieves repletion on a clinically meaningful timeline. For patients whose ongoing blood loss is replenishing depletion as fast as oral supplementation can correct it, oral iron is effectively running in place.
Key Benefits of
IV Iron Infusions
Treats the Real Problem — Not Just the Last Lab Value to Drop: The single most consequential thing Dr. Abdullah does differently in evaluating iron deficiency is running a complete iron panel instead of stopping at hemoglobin. Hemoglobin is the last domino to fall. Ferritin — the body's iron storage protein — depletes first, sometimes dropping to single digits while hemoglobin remains technically within normal range. A woman with a ferritin of 9 ng/mL and a hemoglobin of 12.6 g/dL is profoundly iron deficient by any meaningful clinical definition, with a full symptom burden — crushing fatigue that sleep doesn't fix, cognitive fog, hair shedding by the handful, restless legs at night, cold hands and feet, breathlessness on exertion, and a reduced exercise tolerance she's probably been attributing to being out of shape. She's also been told her iron is fine. Dr. Abdullah checks ferritin, TIBC, transferrin saturation, and hemoglobin every time — because the symptoms that bring patients in follow ferritin, not hemoglobin, and treating by the wrong number means treating people who are genuinely suffering as if nothing is wrong.
100% Bioavailability — The Dose Administered Is the Dose Received: Oral iron absorption under ideal conditions is 10–20% of the administered dose. Under non-ideal conditions — gut inflammation, elevated hepcidin, post-surgical anatomy, individual variability in intestinal transporters — it can be considerably less. Hepcidin, the liver-produced hormone that regulates iron homeostasis, is upregulated by inflammation, infection, and chronic disease — meaning the patients who most urgently need iron repletion are frequently the ones whose oral absorption is most impaired. IV iron bypasses all of this. The iron complex goes directly into the bloodstream, gets taken up by the reticuloendothelial system, and is processed into ferritin and transferrin-bound iron without ever touching the GI tract. The dose prescribed is the dose delivered, full stop. For patients where the math of oral absorption simply doesn't work fast enough or reliably enough, IV isn't a more aggressive version of the same treatment — it's a fundamentally different route with fundamentally different pharmacokinetics.
Eliminates the Tolerability Problem That Makes Oral Iron Fail: Constipation, nausea, heartburn, cramping, metallic taste, dark stools — oral iron at therapeutic doses is genuinely difficult to tolerate for a significant proportion of patients, and the people who need the most aggressive repletion are often the ones taking the highest doses and experiencing the worst GI effects. The clinical consequence is predictable: patients reduce the dose to something tolerable but subtherapeutic, take it inconsistently, or stop entirely — all while technically "on iron therapy." IV iron produces none of these GI effects. Zero. The iron never touches the gut. Patients who've cycled through ferrous sulfate, ferrous gluconate, ferrous bisglycinate, carbonyl iron, and every supposedly gentler formulation on the shelf and still can't tolerate adequate dosing frequently find Venofer infusions completely comfortable. The session itself is sitting in a chair for 30 minutes. Most patients describe it as unremarkable.
Repletes Stores in Weeks, Not Months — Particularly Important When Losses Are Ongoing: For women losing significant iron through heavy menstrual cycles, standard oral supplementation can run in place indefinitely — replacing some of what each cycle takes while the next cycle begins before repletion is anywhere near complete. Ferritin levels drift lower with each cycle while the patient dutifully takes her iron every day and wonders why she isn't improving. A Venofer course of 1,000mg delivered over five sessions doesn't just outpace the losses — it repletes stores on a timeline that produces meaningful symptom improvement within two to four weeks. Energy levels improve. Hair shedding decreases. The cognitive fog begins to lift. Restless legs ease. Most patients describe it as a gradual but unmistakable lifting of a fatigue they had stopped recognizing as abnormal. That's what adequate repletion at a clinically meaningful pace actually feels like — and it's what oral supplementation at standard doses frequently cannot deliver.
Works When Oral Iron Physically Can't — IBD, Post-Bariatric, and Absorption-Impaired Patients: There's a category of patient for whom oral iron isn't just slow or uncomfortable — it's genuinely non-functional. Patients with active Crohn's disease or ulcerative colitis have intestinal inflammation that severely impairs iron absorption while simultaneously causing chronic GI blood loss. Post-bariatric patients who've had Roux-en-Y gastric bypass have altered anatomy that bypasses the duodenum and proximal jejunum — the primary sites of iron absorption — meaning oral iron supplementation after bypass has poor bioavailability even in a healthy gut. Celiac disease produces villous atrophy that reduces absorptive surface area. For these patients, IV iron isn't an upgrade from oral supplementation. It's the treatment that actually works. Dr. Abdullah specifically evaluates absorption status and underlying GI conditions as part of the iron workup, because the treatment plan for a patient with IBD-driven iron deficiency looks meaningfully different from the plan for a patient with dietary iron insufficiency.
Addresses the Neurological and Cognitive Dimension Most People Don't Connect to Iron: Most people associate iron deficiency with being pale and out of breath. The neurological consequences — cognitive fog, poor concentration, word-finding difficulty, mood changes, impaired working memory, and the specific pattern of restless legs syndrome driven by dopaminergic dysfunction in the basal ganglia — are equally real and frequently unrecognized. Iron is a required cofactor in dopamine and serotonin synthesis. Myelin formation and maintenance depends on it. The brain's oxygen delivery is hemoglobin-dependent in ways that affect every aspect of cognitive performance. Patients who've been attributing persistent brain fog to stress, poor sleep, or perimenopause frequently discover after iron repletion that iron deficiency was a significant driver — because the resolution is often rapid and unmistakable enough to establish causation in their own experience. This dimension of iron deficiency treatment is worth naming specifically, because it's one of the most impactful improvements patients report and one of the least anticipated.
Venofer's Safety Profile — Non-Dextran, Six Decades of Clinical Use: The historical concern about serious IV iron reactions was primarily associated with high-molecular-weight iron dextran, a formulation that's largely been replaced by safer alternatives. Venofer is iron sucrose — a non-dextran complex with decades of clinical use across nephrology, obstetrics, gastroenterology, and hematology, with a well-documented safety profile in all of them. Complement-mediated reactions producing transient flushing, warmth, or mild headache are more common than serious hypersensitivity events and resolve without intervention or with minor rate adjustment. Serious reactions are rare and manageable in a clinical setting with appropriate oversight. Every Venofer infusion at Magnolia is administered with a 30-minute post-infusion monitoring period — not because serious reactions are expected, but because physician-supervised medical procedures include the clinical readiness to manage them when they occur.
Who Benefits Most From
IV Iron Infusions
Premenopausal Women with Heavy Menstrual Bleeding This is the patient population most frequently undertreated for iron deficiency, and the one where IV iron produces the most immediate, meaningful clinical impact.
Heavy menstrual bleeding — functionally defined as periods that substantially disrupt quality of life, often with clotting, flooding, or cycles lasting more than seven days — affects roughly one in five women of reproductive age. A single heavy cycle can produce iron losses that take months of consistent oral supplementation to recover from, particularly when the next cycle begins before repletion is complete. For women with fibroids, adenomyosis, endometriosis, or anovulatory cycles driving chronic heavy bleeding, the iron deficit accumulates continuously — faster than oral supplementation can reliably keep pace with.
Many of these women are told their labs are "normal" because their hemoglobin hasn't dropped into the anemic range yet. What frequently isn't measured is ferritin — the storage form of iron. Ferritin can be critically depleted (below 20–30 ng/mL) while hemoglobin remains technically normal, producing the full symptom burden of iron deficiency without meeting the technical definition of anemia. Dr. Abdullah evaluates the complete iron panel — ferritin, TIBC, transferrin saturation, and hemoglobin — specifically because iron deficiency produces symptoms long before anemia does, and treating the complete picture is the clinical standard worth holding to.
Women in Late-Stage Pregnancy Iron requirements increase substantially in the third trimester, and many women approach delivery significantly iron-depleted despite oral supplementation — both because GI tolerance of oral iron is often poor during pregnancy and because fetal demands simply exceed what oral supplementation reliably delivers in the final weeks. Venofer has been used in pregnancy and published data on iron sucrose use during the second and third trimesters has not shown adverse maternal or fetal outcomes. The decision requires individual physician evaluation and gestational age consideration. Dr. Abdullah discusses risk-benefit in detail for pregnant patients.
Patients with Inflammatory Bowel Disease (IBD) Ulcerative colitis and Crohn's disease drive iron deficiency through two simultaneous mechanisms: chronic GI blood loss from mucosal inflammation, and impaired iron absorption from intestinal inflammation that upregulates hepcidin and directly disrupts enterocyte iron uptake. Oral iron also worsens GI symptoms in IBD and can exacerbate mucosal inflammation — making it both less effective and actively counterproductive in many patients. IV iron avoids the gut entirely, making it the preferred approach for iron deficiency in IBD when oral iron has been inadequate or poorly tolerated.
Post-Bariatric Surgery Patients Gastric bypass and sleeve gastrectomy significantly alter GI anatomy and reduce gastric acid production — both essential to effective oral iron absorption. The duodenum, where iron absorption is most efficient, is bypassed in Roux-en-Y procedures. Iron deficiency is nearly universal in long-term post-bariatric patients, and oral supplementation — even with specially formulated products — rarely achieves adequate repletion. IV iron is often the only realistic path to meaningful store restoration in this population.
Patients with Oral Iron Intolerance A significant proportion of patients genuinely cannot tolerate oral iron at doses sufficient for meaningful repletion. GI side effects severe enough to prevent compliance, absorption disorders, or conditions where oral iron's GI effects are clinically unacceptable all represent legitimate indications for IV iron as the appropriate first-choice route — not a second-line option resorted to after prolonged oral failure.
Chronic Kidney Disease (CKD) Iron deficiency in CKD is multifactorial — impaired erythropoietin production, chronic inflammation elevating hepcidin, blood loss from frequent labs and procedures, and reduced intestinal iron absorption all contribute. Venofer has direct clinical trial evidence and long-term real-world use in CKD patients, including those on hemodialysis and peritoneal dialysis, where IV iron is the standard of care.
Restless Legs Syndrome with Low Iron Stores Iron deficiency — even without overt anemia — is strongly associated with restless legs syndrome, and iron repletion consistently improves RLS symptoms in patients with low iron stores. IV iron is appropriate for RLS patients with ferritin at or below 100 ng/mL who haven't adequately responded to or tolerated oral supplementation.
Pre-Surgical Anemia Optimization Iron-deficiency anemia heading into elective surgery increases transfusion risk and impairs postoperative recovery. IV iron before surgery can meaningfully improve preoperative hemoglobin in iron-deficient patients when there's enough lead time for the bone marrow to respond. Dr. Abdullah coordinates pre-surgical iron repletion in consultation with your surgical team's timeline.
What To Expect From
IV Iron Infusions
Step 1 — Iron Panel Labs: Before scheduling infusions, Dr. Abdullah orders a complete iron panel — serum ferritin, TIBC, transferrin saturation, hemoglobin, and CBC. These determine whether IV iron is indicated, estimate how much total repletion is needed, and establish your baseline to track response against. He doesn't infuse iron without confirming deficiency with objective lab data first.
Step 2 — Consultation & Protocol Planning: Dr. Abdullah reviews your symptoms, the underlying cause of your iron deficiency, your relevant medical history, and your medications. He determines your target total iron dose, the number of sessions required, and the spacing between them. For most patients needing full repletion, the typical protocol is five 200mg sessions — often scheduled weekly or biweekly depending on your situation.
Step 3 — Infusion Sessions: An IV catheter is placed in a peripheral vein. Each Venofer session delivers 200mg of elemental iron over approximately 30 minutes. You'll be monitored during infusion and for 30 minutes afterward. Most patients find sessions straightforward — many read, use their phone, or simply rest during the infusion.
Step 4 — Side Effect Profile: Venofer is a non-dextran formulation with a well-documented safety record. The most common side effects — reported in at least 2% of patients in clinical trials — include nausea, headache, dizziness, and transient blood pressure changes. A small number of patients experience GI discomfort, mild arthralgias, or injection site discomfort. Serious hypersensitivity reactions can occur with any IV iron formulation and are the reason post-infusion monitoring is required. Dr. Abdullah's clinical environment has appropriate monitoring protocols and emergency management capability in place for all infusion sessions.
Step 5 — Follow-Up Labs: A complete iron panel and CBC at 4–6 weeks after completing the infusion course confirms the expected response — ferritin rise and hemoglobin improvement if anemia was present. Importantly, transferrin saturation values spike transiently after IV iron due to circulating iron complexes — Dr. Abdullah doesn't check iron studies for at least 48 hours post-infusion to avoid misleading results.
Step 6 — Addressing the Underlying Cause: Iron deficiency has a source, and repletion without addressing ongoing losses means the deficiency will recur. For premenopausal women with heavy menstrual bleeding, Dr. Abdullah discusses management of the underlying menstrual disorder alongside iron repletion. For IBD and CKD patients, IV iron is coordinated with their broader disease management. A maintenance plan is discussed for patients at ongoing risk of re-depletion.

IV Iron Infusions at Magnolia Functional Wellness in Southlake, TX
Iron deficiency doesn't announce itself the way a broken bone does. It creeps in gradually — a little more tired than you used to be, a little less sharp, hair coming out in the shower, reaching for a sweater when nobody else is cold. Most women adapt to it so incrementally that by the time they sit across from Dr. Abdullah and describe their symptoms, they've already normalized feeling this way. That normalization is one of the more frustrating things about iron deficiency, because it's also one of the most treatable conditions in medicine once it's properly identified.
Dr. Farhan Abdullah is a board-certified Internal Medicine physician who sees iron deficiency not as a simple lab value to correct but as a clinical picture to understand — what's driving it, how severely it's affecting you, and what repletion strategy actually makes sense for your situation. At Magnolia Functional Wellness, that means IV iron infusions using Venofer (iron sucrose) for patients where IV delivery is clinically appropriate, alongside an honest evaluation of the underlying cause so the deficiency doesn't simply recur.
Why the Lab Your Doctor Ran May Have Missed It
The single most common reason iron deficiency goes untreated for months or years is incomplete laboratory evaluation. When a physician checks "iron" on a routine panel, they're usually looking at hemoglobin — the measure of red blood cell oxygen-carrying capacity. Hemoglobin is the last thing to fall in iron deficiency. Before hemoglobin drops, your body depletes iron from storage, strips it from non-essential tissue, and conserves it for red blood cell production with remarkable efficiency. You can have a ferritin of 8 ng/mL — essentially no iron reserves — with a hemoglobin of 12.4 g/dL that technically clears the "normal" threshold.
That patient is told her iron is fine. She goes home still exhausted, still losing hair, still craving ice, still dragging through her afternoon. Her iron is not fine.
Dr. Abdullah evaluates the complete iron panel at Magnolia: serum ferritin (the storage marker that falls first), transferrin saturation (how saturated your iron transport protein is), TIBC (total iron binding capacity, which rises as the body upregulates its iron-seeking capacity), and hemoglobin and CBC for the full blood picture. This is the evaluation that actually catches iron deficiency at the stage where patients are symptomatic — not just at the stage where they've become overtly anemic.
Ferritin below 30 ng/mL in the context of symptoms is iron deficiency by any reasonable clinical standard, regardless of what the reference range footer says. Ferritin below 50 ng/mL with low transferrin saturation and symptoms warrants clinical attention. Dr. Abdullah uses these thresholds because that's where patients feel it — not because a lab's reference range tells him to wait longer.
Why IV Iron Instead of Pills
The conversation about oral iron versus IV iron is often framed as a spectrum from least invasive to most invasive — try the pills first, escalate if they don't work. That framing makes sense for some patients and misses the mark entirely for others.
Oral iron requires a functional gastrointestinal absorption pathway. It competes for intestinal transporters that saturate at relatively low doses. It's suppressed by hepcidin — a liver protein that rises in response to inflammation and chronic disease and blocks intestinal iron uptake precisely in the patients who need iron most. It causes nausea, constipation, and GI cramping at the doses needed for meaningful repletion, which is why adherence is notoriously poor. And it's simply slow — restoring depleted iron stores through oral supplementation alone takes months of consistent twice-daily dosing under ideal conditions.
For a woman who loses significant iron every month through heavy menstrual bleeding, oral iron is often running to stand still. By the time one cycle's losses are partially corrected, the next cycle begins. The gap between what oral iron can realistically deliver and what her physiology demands doesn't close.
IV iron with Venofer bypasses the gastrointestinal system entirely. There's no absorption variable, no hepcidin interference, no GI side effects. The iron goes directly into the bloodstream where it's processed and stored or transported to the tissues that need it. Venofer delivers 200mg of elemental iron per session in approximately 30 minutes — a pace that produces meaningful store restoration across a five-session course in a way that months of oral supplementation frequently doesn't.
This isn't about preferring a more dramatic treatment option. It's about matching the intervention to what your physiology actually requires.
The Five-Session Protocol — What It Means in Practice
Venofer's 200mg-per-session dosing means most patients requiring full iron store repletion complete approximately five sessions, typically delivering a total of around 1,000mg of elemental iron. Sessions are generally scheduled weekly or biweekly depending on your schedule and clinical picture.
This is genuinely different from single-visit iron formulations, and worth understanding honestly rather than glossing over. The practical reality at a clinic like Magnolia — where many patients are already coming in for TRT monitoring, GLP-1 follow-ups, IV hydration, or peptide therapy — is that five 30-minute infusion visits over five weeks isn't a significant burden. Each session gives Dr. Abdullah a touchpoint to assess how you're responding, whether symptoms are improving, and whether anything in your clinical picture warrants adjustment.
Response monitoring between sessions also has real clinical value. A patient whose fatigue is lifting noticeably after two sessions is responding as expected. A patient who isn't improving after three may have a more complex picture worth investigating. The structured multi-session protocol creates the monitoring intervals that responsible iron repletion actually requires.
After completing the infusion course, follow-up labs at 4–6 weeks confirm the expected ferritin rise and hemoglobin response. For patients with ongoing causes of iron loss — particularly women with heavy menstrual bleeding — Dr. Abdullah discusses a longer-term monitoring and maintenance plan, because repletion that isn't followed by attention to the underlying problem is just the beginning of the next cycle of deficiency.
Who We See for IV Iron at Magnolia
Magnolia Functional Wellness serves patients from Southlake, Westlake, Colleyville, Keller, Trophy Club, Grapevine, Flower Mound, and throughout the Dallas-Fort Worth area. The patients who most commonly benefit from IV iron infusions include:
Premenopausal women dealing with heavy menstrual bleeding — including those with fibroids, adenomyosis, endometriosis, or cycles that have simply always been heavy — who are exhausted, losing hair, and have been told their iron is "normal" based on hemoglobin alone. Women preparing for or recovering from childbirth with significant iron deficiency. Patients with inflammatory bowel disease who can't absorb or tolerate oral iron adequately. Post-bariatric surgery patients whose altered anatomy makes oral iron absorption unreliable. And patients of any background who have genuinely tried oral iron and found it intolerable at therapeutic doses.
If you've been living with fatigue, brain fog, hair loss, restless legs, or cold intolerance and haven't had a complete iron panel evaluated by a physician who looks beyond hemoglobin alone — that's the right place to start.
How Process Works at
Magnolia Functional Wellness
Assess
We begin with a comprehensive evaluation of your health, goals, and medical background to understand the root causes, not just the symptoms.
Personalize
Based on your results, we create a tailored functional wellness plan using evidence-based therapies designed specifically for your body and needs.
Optimize
Through ongoing care, monitoring, and adjustments, we help you achieve sustainable improvements in performance, vitality, and long-term health.
Complete Iron Panel Evaluation — Not Just Hemoglobin
Dr. Abdullah checks ferritin, TIBC, transferrin saturation, and hemoglobin before any infusion course — because iron deficiency produces symptoms long before hemoglobin drops. Many patients with "normal iron" by incomplete testing are profoundly iron deficient when evaluated properly. The labs come first, every time.
Venofer — Non-Dextran, Decades of Clinical Evidence
Iron sucrose (Venofer) is a non-dextran IV iron formulation with a well-established safety record and long clinical history. It bypasses the GI system entirely, delivers 100% of the administered dose into the bloodstream, and produces none of the GI side effects that make oral iron intolerable for many patients.
The Right Answer for Heavy Menstrual Bleeding
Heavy periods deplete iron stores faster than oral supplementation can reliably restore them for many women — especially when the next cycle begins before repletion is complete. Dr. Abdullah evaluates the complete iron panel and offers IV repletion for women whose clinical picture warrants it, alongside evaluation of the underlying bleeding disorder.
Bypasses Every GI Absorption Barrier
IBD gut inflammation, post-bariatric anatomy, hepcidin upregulation from chronic disease, oral intolerance — IV iron bypasses all of it. For patients whose oral iron absorption is compromised or whose GI tolerance prevents adequate dosing, IV delivery isn't a second-line option. It's often the appropriate first choice.
Physician-Supervised with Proper Post-Infusion Monitoring
Every Venofer infusion at Magnolia is administered with 30-minute post-infusion monitoring and physician oversight. Serious reactions with IV iron are rare but require clinical readiness when they occur. This is a medical procedure supervised by an Internal Medicine physician — not an unsupervised infusion suite.
Treats the Source, Not Just the Symptom
Iron repletion without addressing ongoing losses is temporary. Dr. Abdullah evaluates and discusses the cause of your iron deficiency — heavy menstrual bleeding, GI blood loss, absorption impairment, dietary inadequacy — and builds a plan that addresses the underlying driver alongside the immediate repletion need.
Your Questions Answered
Led by trained medical professionals delivering safe, effective, and scientifically backed aesthetic and wellness treatments.
My doctor told me my iron is normal — why do I still feel exhausted?
This is one of the most common frustrations Dr. Abdullah encounters. When a physician checks "iron," they often mean hemoglobin — the last value to drop in progressive iron deficiency. Ferritin, the stored form of iron, falls long before hemoglobin does. A patient with a ferritin of 9 ng/mL and a hemoglobin of 12.6 g/dL is technically "not anemic" by standard reference ranges but has profound iron store depletion — and experiences the full symptom burden: crushing fatigue, brain fog, hair shedding, cold intolerance, restless legs, and poor exercise tolerance. Dr. Abdullah checks the complete iron panel — ferritin, TIBC, transferrin saturation, and hemoglobin — because treating by hemoglobin alone misses a large portion of symptomatic iron deficiency.
Why can't I just take iron pills?
For some patients, oral iron is entirely appropriate. For others, it simply doesn't work well enough. Oral iron requires functional GI absorption — limited by gut inflammation, hepcidin elevation from chronic disease, post-surgical anatomy, and individual variability. It also requires consistent tolerability, which many patients don't have at therapeutic doses. And for women losing iron each cycle faster than they can replace it orally, supplementation is effectively treading water. IV iron delivers directly into the bloodstream regardless of gut status, produces no GI side effects, and achieves repletion on a timeline that oral supplementation often can't match.
How many sessions will I need?
Most patients requiring full iron store repletion receive a total course of approximately 1,000mg of elemental iron. With Venofer's 200mg-per-session dosing, that's typically five sessions. Dr. Abdullah calculates your individual target dose based on your baseline hemoglobin, ferritin, and weight, and spaces sessions based on your clinical response and schedule. Some patients need fewer sessions; patients with more severe depletion or ongoing losses may need additional courses over time.
Is Venofer safe? I've heard IV iron can cause reactions.
The historical concern about IV iron reactions was largely associated with high-molecular-weight iron dextran — a formulation no longer in common use. Venofer is a non-dextran formulation with decades of clinical use and a well-documented safety profile. Serious hypersensitivity reactions can occur and are the reason all patients are monitored for 30 minutes post-infusion in a clinical setting with appropriate management protocols. Minor complement-mediated reactions — transient flushing, warmth, mild headache — are more common and resolve without intervention or with rate reduction. For the overwhelming majority of patients, Venofer is well-tolerated and uneventful.
How soon will I feel better after iron infusions?
Ferritin begins rising within 24–48 hours of infusion as the administered iron is processed and stored. Hemoglobin improvement in anemic patients typically develops over 2–4 weeks as the bone marrow responds to restored iron availability and produces new red blood cells. Symptom improvement — energy levels, cognitive clarity, reduced hair shedding, restless legs, exercise tolerance — often begins within 1–2 weeks of the infusion course and continues over 4–8 weeks as stores normalize. Most patients describe it as a gradual but unmistakable lifting of a fatigue they had stopped recognizing as abnormal.
Can I get IV iron infusions if I'm pregnant?
Published data on iron sucrose use during the second and third trimesters of pregnancy hasn't shown adverse maternal or fetal outcomes, and Venofer is used in obstetric settings for iron-deficient pregnant patients who can't tolerate or adequately absorb oral iron. The decision is always made on an individual basis, considering gestational age, severity of iron deficiency, and risk-benefit for both mother and baby. Dr. Abdullah discusses this in detail for pregnant patients who inquire.
Why doesn't Magnolia bill insurance for this?
Magnolia Functional Wellness operates as a direct-pay practice — we don't bill insurance for any of our services. This is a deliberate choice that keeps the physician-patient relationship uncomplicated by prior authorization processes, coverage disputes, and reimbursement-driven treatment decisions. Pricing is transparent and available at the front desk. Patients with HSA or FSA accounts may be able to use those funds for IV iron infusions — check with your plan administrator.
Need More Information?
Our team is ready to answer your specific questions and concerns.





Redefine Your Glow. Reimagine Your Life.
Led by trained medical professionals delivering safe, effective, and scientifically backed aesthetic and wellness treatments.
Not what you were looking
for? Explore More.
At Magnolia Functional Wellness, every treatment is guided by medical science, regenerative principles, and individualized care. We focus on restoring physiology at its source, enhancing vitality, and supporting long term health with evidence based interventions that go beyond traditional aesthetics.



.svg)